Explaining the Science: The Potential of Bacteriophages in a Post-Antibiotics World
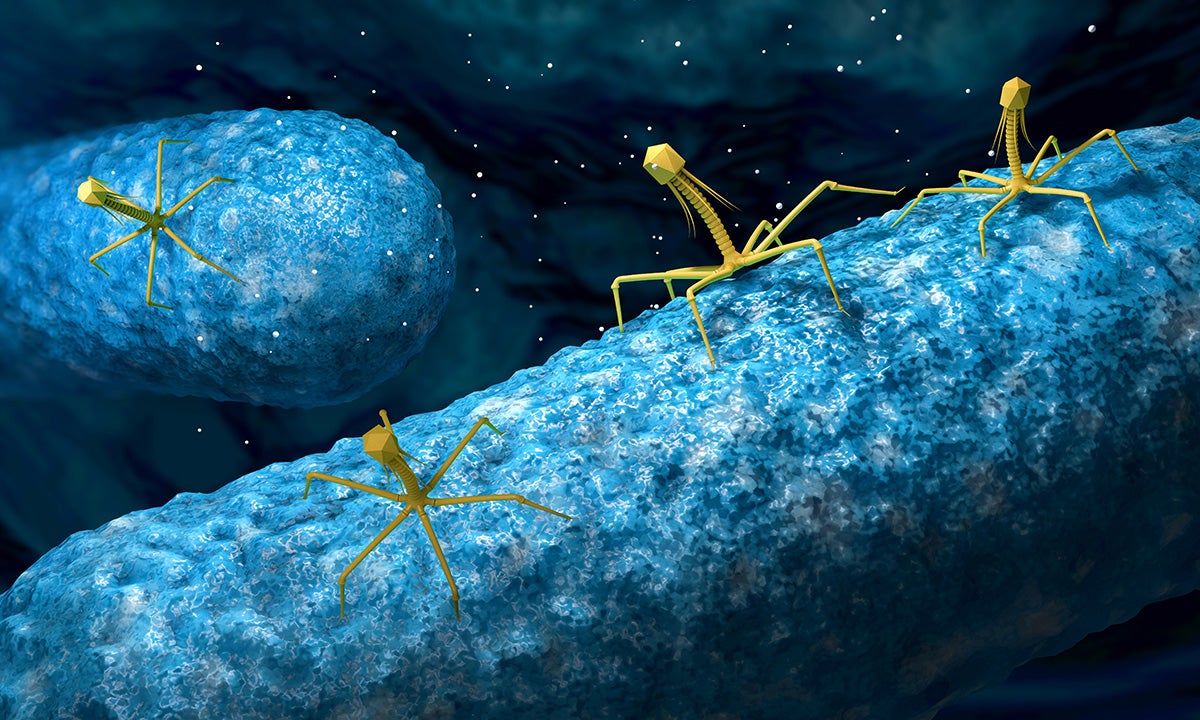
Artist rendering of bacteriophages. Image courtesy of the University of Texas.
As antibiotic-resistant bacteria, like MRSA and resistant strains of tuberculosis and gonorrhea, become more prevalent, health officials are wondering how long antibiotics will be able to hold up against their bacterial foes. And what comes next?
"I don't think we're at the end of the antibiotic era, but we might be close," said the University of Texas at Austin's Ian Molineux. "It's going to take a major rethink of the public health system and a lot of basic research to address."
Some scientists think the answer may lie with a tiny, yet extremely prolific organism: the bacteriophage. The viruses are miniscule biological assassins and they only target bacteria. Recently, doctors have successfully used phages to treat several people who were near death from drug-resistant infections, including two young women with cystic fibrosis, one in England and another in Virginia.
Molineux, a professor of molecular biosciences, has been studying phages for more than 35 years and has spent most of his career focused on understanding the basic biochemical processes at work in phages. In weighing in on the promise and pitfalls of treating infection with phages, Molineux offered five key lessons.
1. Science still has a lot to learn about phages.
In work featured over the summer on the cover of Nature Microbiology, Molineux and his collaborators, describing how the phage P22 infects a type of salmonella bacteria, showed for the first time how a phage of this type is able to get its genetic material past the bacterial cell membranes. Using cryo-electron tomography, researchers found these phages approach bacteria at an oblique angle, rather than attaching vertically like the lunar lander, before the phages orient vertically and attack. It challenged decades of previous thinking about how phages behave.
"It turns out that phages are far more complicated than we give them credit for, and we are still rather ignorant," Molineux said. "I'm just trying to understand very simple, basic biological processes, because if we don't understand them, we're never going to understand anything more complex."
Although skeptical about phages replacing antibiotics altogether, Molineux believes there is a lot of value in basic research to figure out more of the mechanisms phages use to target, infect and destroy bacteria. Drug developers can then explore ways to replicate those mechanisms.
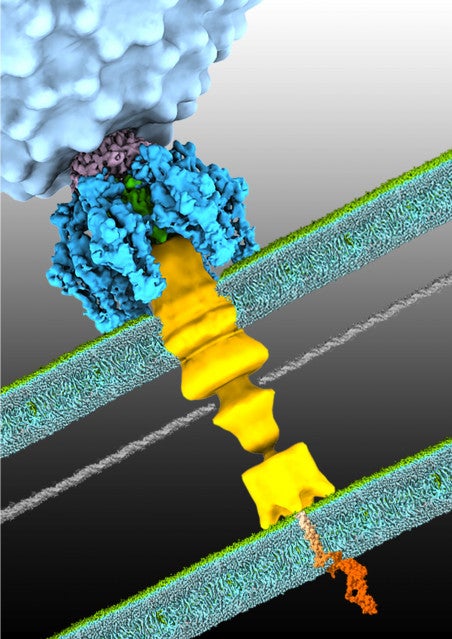
Image of bacteriophage P22 infecting a cell. Image courtesy of Chunyan Wang.
2. Phage treatments aren't as new as the news would you have think.
Phage therapy was discovered about 100 years ago and was one of the only options to treat bacterial infections for decades. The therapy could be hit-or-miss, largely because scientists at the time understood very little about how phages worked. For example, a phage preparation meant to treat cholera in India was preserved using a mercury derivative for the long trip to a hot climate. It turns out, preservative inactivates phages.
When penicillin became commercially available, phage therapy fell out of use quickly and research funding to study phages largely dried up in the 1970s, Molineux explained.
3. The odds are tough for matching bacteria with the right phage.
The challenge with phage therapy is that there are approximately 1031 phages in the world. In order for phage therapy to work, doctors have to use the phage that attacks the specific strain of bacteria infecting a patient.
We only know the detailed biology of perhaps a couple of dozen phages, and even two that are almost identical can have very different therapeutic efficacies. This makes it hard to find a good match.
"There have been some high-profile cases of successful phage therapy, but behind the scenes there was a tremendous amount of work going into finding the right phages. That's just not scalable to large numbers of people. It's not something the average person will be able to use," Molineux said.
4. Just as bacteria adapt to antibiotics, they can adapt to phages, too.
Further complicating the use of phage therapy is the speed at which bacteria can adapt to attacks from phages. Fortunately for infected humans, that often means that bacteria have to ditch genes for antibiotic resistance in the process. And, anecdotally at least, some phage therapy cases have led to antibiotics becoming effective again for those patients.
"Phages are the major driver of bacterial evolution. It's an incredible amount of selection pressure," Molineux says. "Ultimately, it's not the phage or the antibiotic that cures an infection. It's the immune system. If it is not compromised and you give it time to work, by whatever means, it will clear the infection."
5. Even if doctors never widely adopt phages, farmers and ranchers soon might.
Molineux does see one area where pure phage therapy could be useful in curing infections: agriculture. The overuse of antibiotics in livestock and poultry has been linked to antibiotic-resistant superbugs.
"There's been some movement away from antibiotics in agriculture in some countries, and they've seen a significant reduction in antibiotic resistance," Molineux said. "Without the selection pressure, many bacteria will lose the resistance."
Molineux has studied a phage therapy used on dairy cows in the Republic of Georgia, where there was evidence that nearly all of the animals were cured of mastitis, a bacterial infection that interferes with milk production. Choosing the "right" diseases to treat, and learning how to select the "right" phages may ultimately provide a clear path to routine phage therapeutic applications.